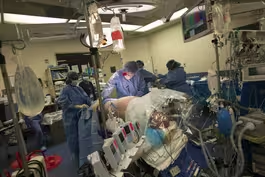
West Virginia doctors work to bridge rural healthcare gap
Clip: 3/22/2023 | 9m 3sVideo has Closed Captions
West Virginia doctors work to bridge healthcare gap in rural areas
When it comes to health, rural America lags far behind the country’s urban and suburban areas. The reasons are complex and these challenges are the focus of a new series called Rural RX. With support from the Pulitzer Center and in collaboration with the Global Health Reporting Center, William Brangham starts our series in Martinsburg, West Virginia.
Problems playing video? | Closed Captioning Feedback
Problems playing video? | Closed Captioning Feedback
Major corporate funding for the PBS News Hour is provided by BDO, BNSF, Consumer Cellular, American Cruise Lines, and Raymond James. Funding for the PBS NewsHour Weekend is provided by...

West Virginia doctors work to bridge rural healthcare gap
Clip: 3/22/2023 | 9m 3sVideo has Closed Captions
When it comes to health, rural America lags far behind the country’s urban and suburban areas. The reasons are complex and these challenges are the focus of a new series called Rural RX. With support from the Pulitzer Center and in collaboration with the Global Health Reporting Center, William Brangham starts our series in Martinsburg, West Virginia.
Problems playing video? | Closed Captioning Feedback
How to Watch PBS News Hour
PBS News Hour is available to stream on pbs.org and the free PBS App, available on iPhone, Apple TV, Android TV, Android smartphones, Amazon Fire TV, Amazon Fire Tablet, Roku, Samsung Smart TV, LG TV, and Vizio.
Providing Support for PBS.org
Learn Moreabout PBS online sponsorshipEOFF BENNETT: When it comes to health, rural America lags far behind the rest of the country.
The reasons are complex, from demographics, to doctor shortages, to the sheer distances that many people have to travel to see a provider.
These challenges are the focus of a series we start tonight.
With support from the Pulitzer Center and in collaboration with the Global Health Reporting Center, William Brangham reports from West Virginia for our series Rural Rx.
ANGIE GRAY, Berkeley Medical Center: And this is where I grew up.
I have lived in Morgan County my entire life.
We're up here on a mountain.
You're an hour from your nearest Walmart.
So, some people may not want to live that way.
But, to us, this is home.
WILLIAM BRANGHAM: This mountain, this slice of West Virginia has been home to nurse Angie Gray's family for six generations.
ANGIE GRAY: Hey, Erin (ph).
Hi, Patti (ph).
WOMAN: Hi.
WILLIAM BRANGHAM: Gray is visiting a family friend, Patti, who has chronic obstructive pulmonary disease.
She struggles to afford her medications and cannot live without her oxygen.
The power at their house is unreliable, so there's a generator at the ready so Patti can always breathe.
WOMAN: It's hard finding someone good around this area to help you.
ANGIE GRAY: Yes.
WILLIAM BRANGHAM: Gray says these kinds of struggles are everywhere here.
ANGIE GRAY: So, that might be an option that can help.
We take care of our own.
I always say that West Virginians are all connected.
We're all family.
But, really, my mission is to advocate for people who are so vulnerable that they don't have a voice.
When you look at West Virginia specifically, we have the highest numbers of chronic disease, diabetes, heart disease.
We're losing so many of our people to death, and early to death.
WILLIAM BRANGHAM: On nearly every health metric, rural America fares worse than the rest of the country, from life expectancy to maternal mortality.
Compared to urban areas, rural residents are a third more likely to die of diabetes, about 20 percent more likely to die from heart disease, and more likely to die of cancer or accidents.
There are higher smoking rates here and fewer people with health insurance.
In many health categories, West Virginia, a heavily rural state, ranks dead last.
These are the challenges that Dr. Michael Londner and his colleagues face.
He's chairman of the emergency department at Berkeley Medical Center in Martinsburg.
DR. MICHAEL LONDNER, Berkeley Medical Center: For as many of the myths there are, some of those myths are not urban legends.
They're reality.
The idea that someone waited four days having a heart attack at home because they couldn't get transportation, and they wouldn't call 911 because it cost too much, even though it's free in most of the regions.
But they don't know that.
WILLIAM BRANGHAM: People in rural areas are less likely to have access to good-quality health care.
Compared to urban areas, rural America has fewer nurses and fewer than half as many doctors per person.
People have to go farther to access care, unless they have someone like Angie Gray to help them.
ANGIE GRAY: So, if you already struggle for transportation, or you live in a more rural area that's going to take you an hour to access health care, some places in West Virginia two hours to access health care, you're less likely to make it there.
And it can help.
WILLIAM BRANGHAM: When people do come for care, they're often using the emergency room as a doctor's office, something Dr. Londner and his team have turned into a virtue.
DR. MICHAEL LONDNER: For a lot of those folks, we can actually use our emergency department sort of as a primary care office sometimes.
And so a number of those people are here with kids with fevers.
So we're giving antipyretics and we're doing swabs.
Why do you need to be in a room doing that?
And, on any given day, you have three rooms with 8-year-olds that have flu, two overdoses, and then five people who are elderly and looking for admission because their chronic diseases.
WILLIAM BRANGHAM: In some cases, he says, that emergency room visit is the first time a patient has seen a doctor in their entire life.
DR. MICHAEL LONDNER: Some of the folks I see have never had health care ever, and they're in their 60s or 70s.
WILLIAM BRANGHAM: Never had health care... DR. MICHAEL LONDNER: Ever.
WILLIAM BRANGHAM: ... meaning they don't have a doctor?
DR. MICHAEL LONDNER: Correct.
Not only do they not have a doctor.
They may not have had one as a kid growing up.
They may have never been vaccinated.
For them, the opportunity might -- just to meet a physician for the first time.
Or they come in and you say, do you have any history of high blood pressure, diabetes, things like that?
They're like no.
And they're hypertensive.
Their sugar is 400.
And you're like, oh, you have never been tested before, so you don't know that you have those things.
WILLIAM BRANGHAM: Not going to the doctor for preventive care is not uncommon in parts of West Virginia, a pattern that is repeated across rural America.
DR. MICHAEL LONDNER: If you want someone to come to the hospital, you have probably got to get them here.
If you're going to put them on dialysis, and they can't go, you might as well not write the prescription.
If you're going to give them $700 worth of antibiotics or hypertensive medicine, just realize they're going to throw it away, because they can't afford it.
I felt like places I had been in the world doing disaster work were better off than certain people who lived here.
A certain percentage of my people don't have indoor plumbing still.
Access to power in certain regions here is still not 100 percent available.
There's a lot of places that we have ambulances go into, and they show up here, and they're like, I don't know if they're going to have a medical problem, but you can't send them back to that.
And you're like, to what?
And they will show you pictures of, they're living in a place that is rat-infested.
There's raccoons inside the house.
There's feces everywhere.
Like, this is where they live.
And this is the best they can do.
DR. MADISON HUMERICK, West Virginia University Medicine: We go out and meet them where they are.
WILLIAM BRANGHAM: Since getting to a hospital or a clinic can be difficult for so many, Dr. Madison Humerick goes to them, delivering preventive and essential care straight out of her toolbox.
DR. MADISON HUMERICK: It looks like you have had ear infections in there before, huh?
WOMAN: Yes.
DR. MADISON HUMERICK: We probably prevented a couple urgent care visits today with this.
WILLIAM BRANGHAM: Is that right?
DR. MADISON HUMERICK: Oh, yes.
It was awesome.
I mean, we got to prescribe some antibiotics.
So, it was convenient for them.
We're just going right back to old-school family medicine, which is what we love.
WILLIAM BRANGHAM: Urgent care out in the open.
DR. MADISON HUMERICK: Urgent care out on the street, yes.
WOMAN: Pain recovery.
This is Jamica (ph).
WILLIAM BRANGHAM: At times, practitioners here say the need can be overwhelming, especially when it comes to mental health.
Rural Americans report higher levels of depression and suffer suicide rates more than 30 percent higher than people who live in cities.
And yet, for those people, it's harder to find help.
Rural areas have fewer than half as many psychologists per capita.
SAMANTHA DEAMER, West Virginia University Medicine: That means that we have a year-plus wait-list in our outpatient clinic.
It was recently two years.
I think we have gotten that down to a year-and-a-half for adults.
WILLIAM BRANGHAM: Dr. Samantha Deamer is a clinical psychologist who works out of the Harpers Ferry Family Medicine Center.
In atypical fashion, she embeds with this family practice to make it seamless for patients who want mental health care.
But, elsewhere, people face big obstacles.
SAMANTHA DEAMER: That mean, for kids, they're waiting a year-plus for specialty services, like testing for ADHD or developmental disabilities.
Our neuropsychologist wait-list is incredibly long.
So, just a lack of available services overall.
WILLIAM BRANGHAM: So people who could be in a in a crisis-like circumstance... SAMANTHA DEAMER: Yes.
WILLIAM BRANGHAM: ... would call and say, "Hey, can I get help?"
and they're told?
SAMANTHA DEAMER: Go to the emergency room, because that's all we can offer, yes.
ANGIE GRAY: Can you start browning the chicken while I get the vegetables cut up?
MAN: Yes, I can.
ANGIE GRAY: OK. WILLIAM BRANGHAM: We caught back up with nurse Angie Gray after she visited her friend, Patti.
How typical is that circumstance of what we saw today?
ANGIE GRAY: Typical, very typical, yes.
A lot of people that I know personally, a lot of patients that we have, they're all dealing with that, trying to be able to afford to get their medications, trying to get to good health care.
WILLIAM BRANGHAM: Hoping the power stays on.
ANGIE GRAY: Hoping the power stays on, so that you're not out of your oxygen.
WILLIAM BRANGHAM: Gray says these problems are ultimately fixable, but not if we tackle them piecemeal, one patient at a time.
ANGIE GRAY: There's a parable in public health.
There's a villager who walks up to the river and there's a baby floating down the river.
So he pulls the baby out.
Another ones comes floating down the river, so he pulls the baby out.
All the villagers are gathering around the river.
And all these babies start coming down the river, and they're jumping in, pulling them out, until one villager walked upstream to see who was throwing the babies in the river.
And we need to get more upstream.
WILLIAM BRANGHAM: Gray admits it's an uphill climb, but it's one they're taking step by step.
For the "PBS NewsHour," I'm William Brangham in rural West Virginia.
Baseball's new pitch clock speeds up the game
Video has Closed Captions
Baseball's new pitch clock speeds up the game, draws mixed reaction from players and fans (5m 19s)
Fed raises interest rates again in wake of bank failures
Video has Closed Captions
Fed raises interest rates again in wake of bank failures (8m 3s)
'From Generosity to Justice' proposes shift in giving
Video has Closed Captions
Darren Walker proposes shift in focus of giving in new book 'From Generosity to Justice' (7m 41s)
Government announces organ transplant system overhaul plan
Video has Closed Captions
Biden administration proposes overhaul of organ transplant system (6m 15s)
Political ramifications of Trump's legal troubles
Video has Closed Captions
How Trump's possible indictments will influence Republican political strategy (7m 10s)
Supreme Court hears case involving Jack Daniel's and dog toy
Video has Closed Captions
Supreme Court hears trademark case involving Jack Daniel's and dog toys (4m 38s)
Providing Support for PBS.org
Learn Moreabout PBS online sponsorship
- News and Public Affairs
Today's top journalists discuss Washington's current political events and public affairs.

- News and Public Affairs

FRONTLINE is investigative journalism that questions, explains and changes our world.












Support for PBS provided by:
Major corporate funding for the PBS News Hour is provided by BDO, BNSF, Consumer Cellular, American Cruise Lines, and Raymond James. Funding for the PBS NewsHour Weekend is provided by...